Largest ever UK surgical trial aims to reduce post-surgery infections
More than £10m of funding from the National Institute for Health and Care Research (NIHR) has been awarded to BHP founder-member the University of Birmingham to run an ambitious trial which aims to recruit 26,000 patients from 100 sites across the UK in the next five years.
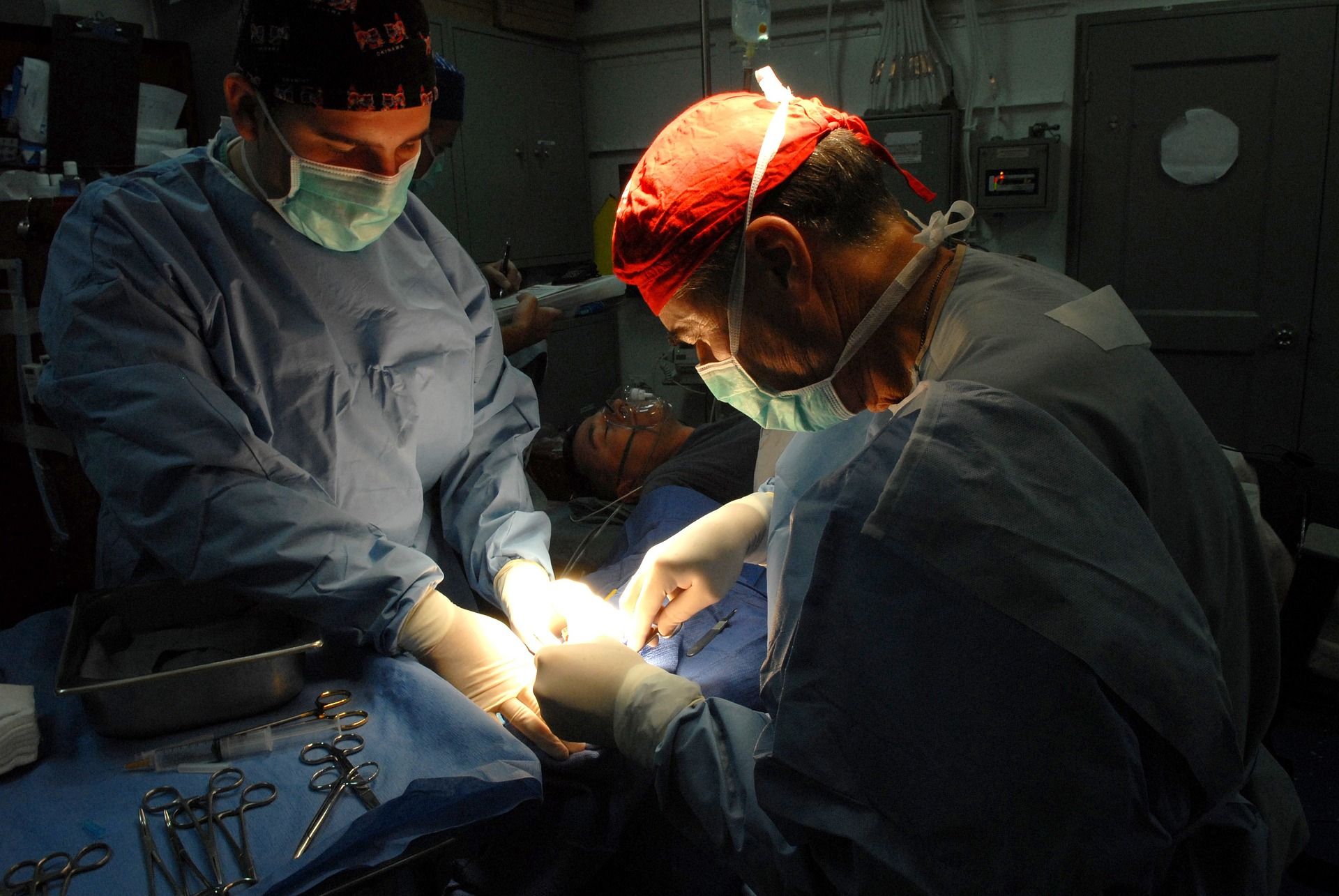
ROSSINI-Platform is a large multi-arm, multi-stage platform trial, led by Professor Thomas Pinkney and the Birmingham Clinical Trials Unit, that will help experts understand how to reduce wound infections that can occur following operations.
Wound infections, also referred to as Surgical Site Infections (SSI), are the commonest complication after surgery and affect up to one in four patients undergoing surgery each year. These infections carry an estimated cost to the NHS of at least £700m each year.
Professor Thomas Pinkney from the School of Health Sciences at the University of Birmingham, and Chief Investigator of the ROSSINI-Platform trial said: “An adult living in the UK will have an average of four operations during their lifetime. Up to a quarter of operations may result in a surgical site infection (SSI) – a post-operative infection of the wound – which can have significant negative impacts on patient recovery.
“We know that infections at different operation sites can cause different types of challenges. For example, an infection following a caesarean section can impact on the mothers’ ability to bond with their newborn. An infection following amputation could mean that the patient is no longer suitable to be fitted for a prosthetic, meaning they might become a wheelchair user.
“Post pandemic the waiting lists for surgeries are higher than ever, so an evidence-based approach to improving recovery times and reducing preventable complications and their associated risk of readmissions has never been more necessary.”
ROSSINI-Platform will look at various interventions to reduce the rates of surgical site infection, and the design of the trial will enable the team to focus on those that show evidence of benefit.
In total, 18 interventions are being assessed in the trial, with examples including:
- using state-of-the-art wound cleaning solutions during surgery
- using special wound dressings after surgery,
- applying antibiotics differently during surgery,
- changing gloves and instruments at certain points during surgery,
- waxing or epilation around the surgical site
In addition, the trial will test these interventions across multiple operation types areas such as heart surgery, brain surgery, caesarean section and leg amputation, to find what works best to reduce infection in each setting.
Sue’s story
Sue Blackwell, 49, from Liverpool, has faced health issues over the years connected with inflammatory bowel disease and has had a total of 13 operations. Several operations have resulted in SSIs requiring antibiotics, but one infection led to unexpected complications that impacted Sue’s life for years.
Following a planned completion proctectomy, Sue developed a serious infection leading to being housebound for six months and losing control of her bladder for ten weeks.
Sue had to wait for district nurses to come and change her dressings twice each day, and this had a significant impact on her life. To add to the ordeal, Sue had to undergo additional surgeries to address the complications and experienced problems with wound draining for two years. The seemingly never-ending round of surgeries and treatments continued, and it took a total of eleven years for the wound to fully heal.
Sue is currently doing a PhD at the University of Birmingham and will use her lived experience to inform the ROSSINI-Platform trial as a public involvement representative.
Speaking of her involvement in both developing and delivering the study, Sue said:
“A lot of patients think that someone somewhere along the line is at fault, which isn’t usually the case. SSIs are very common and we don’t know enough about what we can do to stop them. With this trial, all the interventions are already in use, we know they are all safe, we’re just testing them against each other in a smart way, similar to a world cup tournament, to see which comes out on top.”
In addition to delaying or impeding patient recovery, SSIs are responsible for extending hospital stays and hospital readmissions. SSIs are a significant problem for the NHS, due to increased treatment costs and resource usage both in hospital and in the community. SSI is now the most common healthcare associated infection and costs the NHS at least £700million per year. It is therefore a priority for patients and the health service.
The trial team hope that the findings will help countries around the world to implement the most effective ways to prevent SSI following different types of common surgeries. This will help speed up recovery, get patients discharged from hospital sooner freeing up bed space, and in many countries around the world will save countless lives.